The Complete Guide to Healthcare Software Development in 2026
Healthcare software development in 2026 is not a single discipline. It is six distinct product categories, each with its own compliance perimeter, integration burden, and cost curve.

Acquaint Softtech
Most briefs that reach Acquaint Softtech for healthcare software development are scoped at half their actual cost. Compliance is added at the end instead of designed in on day one, and teams are planned as engineers only, missing the compliance, security, and clinical roles the work actually needs.
The result is predictable: six-figure compliance rework, missed launches because audit logs were not specified, EHR integrations stalled because HL7 versus FHIR was decided too late, and vendor changes mid-build because domain depth was never there.
According to HHS Office for Civil Rights enforcement data, breach settlements in this category routinely run into seven figures, and a meaningful share originate in vendor systems.
This healthcare software development guide 2026 fixes that gap with an operator-level roadmap drawn from real delivery. Acquaint Softtech is an Official Laravel Partner with 70+ engineers, 1,300+ projects shipped over 13 years, and 48 verified Clutch reviews; our healthcare practice covers telemedicine, EHR, RPM, hospital systems, pharmacy, and clinical AI.
- Founders evaluating a healthcare software build for the first time and trying to scope cost, compliance, and timeline.
- CTOs and engineering leads at hospitals, clinics, or HealthTech startups comparing in-house build versus outsourced delivery.
- Product managers planning a telemedicine, EHR, RPM, or pharmacy product and selecting a primary tech stack.
- COOs and operations heads building a vendor framework for an ongoing healthcare software development programme.
You can start with our custom software product development approach if you want a single end-to-end engagement. Every cost, timeline, and compliance benchmark below comes from shipped work, not theory.
Healthcare Software Market in 2026: What's Driving Demand
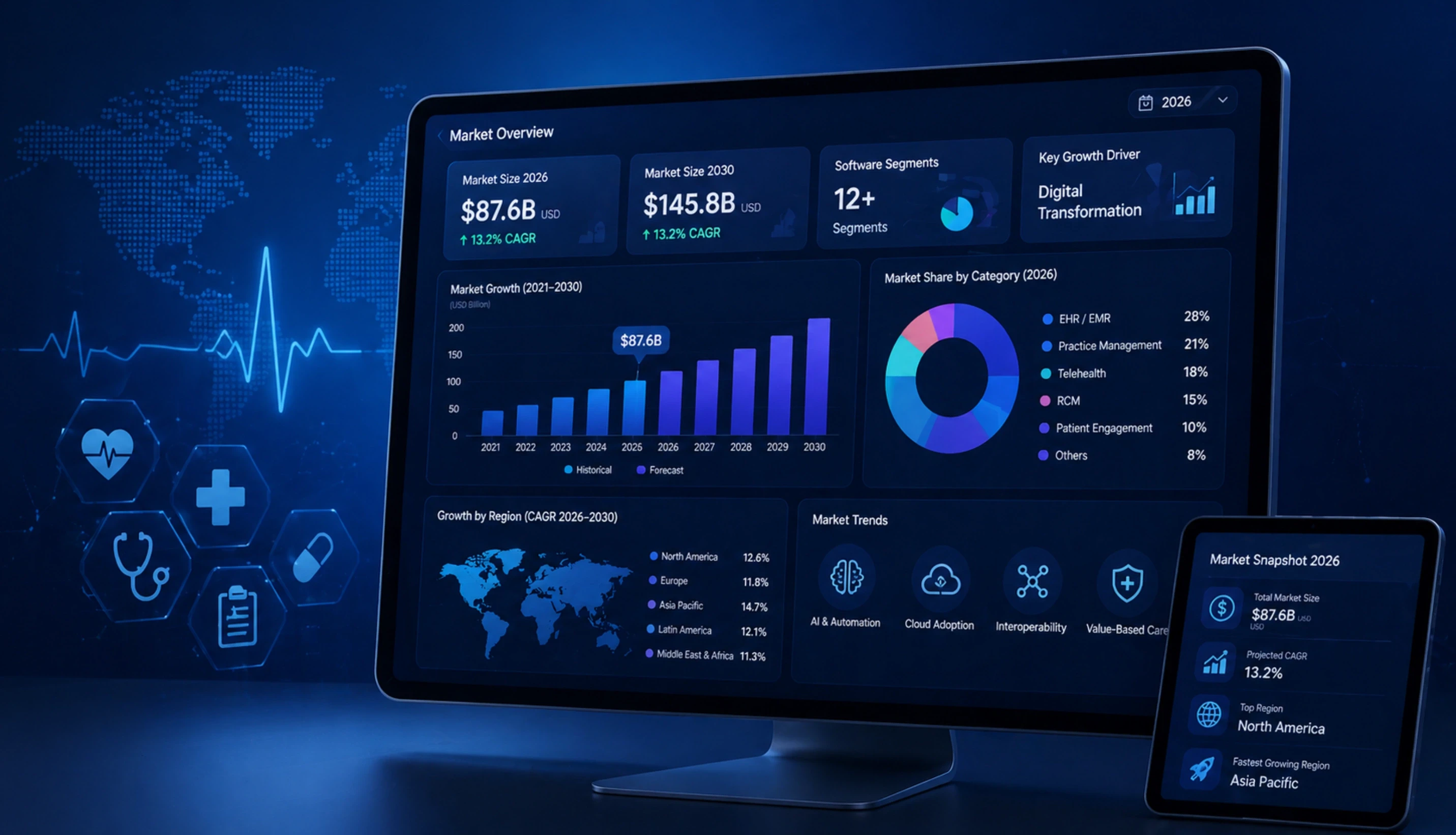
Before scoping a healthcare software build, it is worth understanding the market context in which the product will land. The 2026 healthcare software market is being reshaped by four converging forces, and each one is creating distinct categories of buying demand that map directly to the build decisions later in this guide.
Force 1: Post-pandemic virtual care has stabilised as a permanent channel
Telemedicine usage is no longer a pandemic spike. Across 2024 and 2025 it settled into a baseline of 15 to 25 percent of total clinical encounters in mature markets, depending on the specialty. Mental health, primary care, and chronic disease management lead the share; surgical specialties remain primarily in-person.
The implication for software buyers: virtual care is now treated as a permanent product investment rather than an emergency tool, which means buyers expect production-grade compliance, EHR integration, and clinician workflow polish from the outset. The throwaway pandemic-era video tools are being replaced with proper systems. Among the durable benefits of healthcare software development at this maturity stage: lower clinician minutes per encounter, measurable reduction in no-shows, and a cleaner audit trail than paper-anchored workflows ever produced.
Force 2: Reimbursement pressure is forcing operational digitisation
US Medicare's expansion of remote patient monitoring (RPM) reimbursement codes (CPT 99453, 99454, 99457, 99458) and chronic care management codes has made device-driven care commercially viable for clinics that could not previously afford the staff overhead. Equivalent shifts in the UK NHS, Australia's MBS, and the UAE's DHA are creating parallel demand.
The implication: there is real, sustained buying demand for RPM platforms, chronic care management tools, and the integrations that connect them to billing systems. Healthcare software market trends 2026 favour products that close the loop from clinical event to billable claim.
Force 3: AI-assisted clinical workflow is moving from pilot to production
Ambient scribing tools (the AI-assisted clinical note generation category) crossed from pilot to standard offering in 2024 and 2025 across major US health systems. Diagnostic image analysis for routine reads (chest X-ray triage, retinal screening, dermatology pre-screen) is following the same pattern.
The implication: healthcare software now usually includes at least one AI feature. Acquaint Softtech delivers this work through our
practice, with most engagements integrating large language models for documentation tasks and narrower task-specific models for diagnostic support.
Force 4: Regulatory enforcement is tightening
HIPAA enforcement action volume rose materially across 2024 and 2025, with several settlements in the seven-figure range for breaches that originated in vendor systems. UK and EU regulators have continued tightening Data Protection Impact Assessment (DPIA) expectations under GDPR. The UAE Federal Health Data Law has moved from publication to active enforcement.
The implication: healthcare software buyers are scrutinising vendor compliance discipline more carefully than they did three years ago. A vendor without documented HIPAA controls, a recent penetration test, and Business Associate Agreement (BAA) infrastructure is no longer competitive for serious procurement processes.
What this means for healthcare software demand in 2026
These four forces produce a market where the most common active buying conversations Acquaint Softtech has with new prospects fall into four shapes: virtual care platform builds (Force 1), RPM and chronic care platforms (Force 2), AI-feature additions to existing healthcare products (Force 3), and compliance retrofits or modernisation projects (Force 4). All four require the same underlying engineering discipline. The differences are in scope, integration, and time horizon.
Stepping back, this is also why businesses need healthcare software development as a strategic capability rather than a one-off project. The market is no longer rewarding one-shot builds that ignore reimbursement codes, AI integration, or evolving regulatory enforcement. It is rewarding systems that ship, then iterate against real clinical and billing data over multi-year horizons. The vendor relationship that supports that iteration matters more than any single launch milestone.
Quick Take
Four forces are shaping demand in 2026: stable virtual care, RPM reimbursement codes, AI moving to production, and tighter regulatory enforcement. The buying conversation is now about durable, multi-year systems, not one-shot builds.
Map Your Product to Market Forces →
What Healthcare Software Actually Is: The Six Categories

Healthcare software is any system that captures, processes, transmits, or analyses health-related data for clinical, administrative, or patient-facing use. Across our 1,300+ delivered projects at Acquaint Softtech, healthcare engagements consistently fall into six distinct categories that differ by user, by integration surface, and by regulatory weight.
Understanding which category your product belongs to is the single most important early decision. It determines the team you need, the integrations you must build, the regulators you answer to, and the cost. Some products span two categories; where they do, the higher-compliance category sets the standard for the entire system.
Telemedicine and Virtual Care Platforms
Telemedicine systems connect a patient and a clinician in real time over video, audio, or asynchronous messaging. The engineering perimeter is small in code volume but heavy in real-time infrastructure: WebRTC or Twilio for video, end-to-end encryption for media streams, calendar and payment integration, and electronic prescribing where the jurisdiction allows.
The clinical record is usually thin and the compliance focus is on session encryption, identity verification, and audit logs. Telemedicine builds tend to be the fastest healthcare engagements to ship, with MVPs landing in 16 to 22 weeks. They are also the most commonly underestimated, because the visible video-call surface obscures the back-end work in scheduling, eligibility, and prescription routing.
Common buyers: HealthTech startups, specialty practice groups, mental health platforms, and hospital virtual care divisions.
Electronic Health Records and EHR Modules
An EHR is the longitudinal clinical record of a patient: encounters, diagnoses, medications, allergies, lab results, imaging references, vitals, and workflows related to healthcare chart abstraction for clinical review and reporting. EHR builds carry the heaviest data model in healthcare software and the largest interoperability burden. Health Level 7 version 2 (HL7 v2) and Fast Healthcare Interoperability Resources release 4 (FHIR R4) are the two interfaces every modern EHR exposes.
Custom EHR work usually replaces an off-the-shelf product that has hit a workflow or cost ceiling, and the rebuild has to support data migration from the legacy system without losing the audit trail. Greenfield EHR builds are rare because the regulatory bar is high and the off-the-shelf incumbents (Epic, Cerner, Athena) hold the market for general-purpose use.
Common buyers: specialty practices that off-the-shelf EHRs serve poorly (mental health, dermatology, fertility, addiction medicine), hospital networks consolidating multiple acquired systems, and HealthTech vendors building EHR-adjacent workflow tools that integrate with the major incumbents through FHIR.
Remote Patient Monitoring and Connected Devices
RPM platforms ingest readings from wearables, glucose meters, pulse oximeters, ECG patches, and other connected medical devices. They route alerts to clinicians and bill against Current Procedural Terminology (CPT) codes such as 99453, 99454, and 99457 in the US market. The engineering split is roughly two-thirds backend and one-third frontend: device protocols, time-series storage, alert engines, and reimbursement logic dominate the work.
Frontend is typically a clinician dashboard plus a thin patient app. The technical complexity sits in three places: the device-integration layer (Bluetooth Low Energy, manufacturer SDKs, FHIR Device profiles), the time-series ingestion and alerting backbone, and the billing event generation that maps clinical events to CPT codes the practice can submit.
Common buyers: cardiology and chronic-disease management companies, home-health agencies, value-based-care organisations operating risk contracts, and connected-device manufacturers building the software side of their hardware product.
Hospital and Clinic Management Systems
Hospital information systems (HIS) and clinic management platforms cover scheduling, billing, inventory, bed management, pharmacy, lab order routing, and revenue cycle. These are the largest healthcare software builds by surface area and the most operationally invasive: the system replaces the operational nervous system of the institution.
Replacing an existing HIS is rarely a single build; it is a multi-year programme with phased cutover, parallel running, and continuous integration with finance and HR systems.
Common buyers: mid-size hospitals replacing aged in-house systems, specialty clinic chains scaling beyond what their original software supports, and emerging-market hospital networks where off-the-shelf US options price out.
Pharmacy, Lab, and Diagnostics Software
Pharmacy management systems handle prescription verification, drug interaction checks, inventory, controlled substance tracking, and insurance claims. Lab information systems (LIS) handle order entry, sample tracking, instrument interfaces, and result delivery to ordering clinicians. Diagnostics platforms add imaging workflow, structured reporting, and Picture Archiving and Communication System (PACS) integration.
All three sub-categories carry specific regulatory regimes that go beyond general healthcare privacy law. Drug Enforcement Administration (DEA) controls apply in the US for controlled substances. GDPR plus national rules apply across the EU. Lab systems intersect with Clinical Laboratory Improvement Amendments (CLIA) in the US and ISO 15189 internationally. Imaging platforms touch Digital Imaging and Communications in Medicine (DICOM) standards and, where used for diagnosis, US Food and Drug Administration (FDA) Software as a Medical Device (SaMD) classification.
Common buyers: independent pharmacy chains, lab networks scaling beyond legacy systems, hospital diagnostic departments, and HealthTech vendors building specialised reporting or workflow tools that integrate with the major lab and imaging incumbents.
AI, Analytics, and Clinical Decision Support
This category is the fastest-growing in the 2026 market: clinical decision support tools, diagnostic image analysis, predictive readmission models, ambient scribing, and AI-assisted coding. The engineering challenge is less about model training and more about integration, governance, and explainability.
A useful clinical AI feature is one that fits a clinician's existing workflow, exposes its reasoning, and degrades gracefully when the model is uncertain. It is not a generic chatbot bolted onto a chart. The successful patterns we have shipped at Acquaint Softtech are narrow, well-scoped, and instrumented for outcome measurement from day one.
Quick Take
Healthcare software splits into six categories: telemedicine, EHR, RPM, hospital management, pharmacy/lab/diagnostics, and clinical AI. Pick the category first; the team, integrations, regulators, and cost all derive from it.
Acquaint Softtech delivers all six categories through our software product development services practice. The category-specific delivery teams pull from a 70+ engineer bench, with healthcare-experienced tech leads who have shipped at least one production system in the relevant category.
Healthcare Software vs General SaaS: The Structural Difference
Founders coming from a general SaaS background often estimate healthcare projects using SaaS benchmarks. The estimates are wrong by a factor of two to three because healthcare carries five structural costs that SaaS does not. The table below shows the differences side by side.
Dimension | General SaaS Build | Healthcare Software Build |
Compliance burden | GDPR or local privacy laws apply to most data fields; controls are documented but not externally audited. | HIPAA, HITECH, GDPR, and country-specific medical-device regulations apply; controls are externally audited and breach notifications are mandatory. |
Audit trail | Optional; usually limited to admin actions and security events. | Mandatory and immutable; every read, write, and export of a clinical record must be logged with user, timestamp, and reason. |
Integrations | REST APIs to a handful of third-party services like Stripe, Twilio, or Salesforce. | HL7 v2 and FHIR R4 to one or more EHRs, DICOM to imaging systems, device protocols for RPM, and payer APIs for claims. |
Testing burden | Unit, integration, and end-to-end automated tests cover most paths. | All of the above plus clinical workflow validation, edge case testing for safety, and a documented test evidence trail for audit. |
Hosting and infrastructure | Any major cloud region; cost optimised for performance. | HIPAA-eligible cloud regions with Business Associate Agreements; encryption at rest and in transit; isolated environments per tenant where required. |
Build timeline | MVP in 8 to 12 weeks is realistic for a focused scope. | MVP in 16 to 24 weeks is realistic for a focused scope, with compliance documentation running in parallel. |
Team composition | Frontend, backend, devops, QA. | All of the above plus a compliance lead, a clinical advisor or domain SME, and a security engineer for production deployment. |
The principle: healthcare software is not SaaS with an extra checkbox. It is SaaS with a parallel compliance programme running through every sprint.
Acquaint Softtech runs that parallel programme as a standard part of every healthcare engagement. That is why our healthcare clients deploy production-ready systems rather than systems that need a six-month compliance retrofit before launch. The compliance documentation set is built incrementally, sprint by sprint, alongside the code, not bolted on at the end.
The structural overhead of healthcare also affects how to think about the team. A SaaS team of four developers can ship a credible MVP in three months. A healthcare team of four developers will ship slower, not because the developers are slower, but because the work itself includes audit log design, encryption review, BAA negotiation with the cloud provider, and integration with at least one external clinical system.
If your team has not delivered a HIPAA-aligned build before, the lower-risk path is a dedicated software development team with a tech lead who has shipped healthcare software in the same category.
How a Healthcare Software Build Actually Works: Phase by Phase
Founders ask us how to build healthcare software end-to-end without skipping the steps that healthcare specifically requires. The answer is the five-phase delivery shape below, a step by step healthcare software development model we use across every healthcare engagement at Acquaint Softtech, regardless of category.
Across our healthcare delivery operations, a build runs in five named phases. The phase names below match what appears on Acquaint Softtech project plans and what the client signs off on at each stage. Each phase has a clear entry condition, a clear deliverable, and a clear exit. Clients can pause the engagement at the end of any phase, which is what makes the model risk-adjusted for both sides.
Phase 1: Discovery and Compliance Scoping
The product manager, the client clinical lead, and the Acquaint tech lead define the scope, the data model, and the compliance perimeter. The output is a written specification that names every Protected Health Information (PHI) field the system will store, every external integration, every user role, and the regulatory regime the build will satisfy.
No code is written in this phase. The client signs the specification before Phase 2 begins. This is also where the BAA conversation with the chosen cloud provider starts, where the clinical advisor (if external) is engaged, and where any third-party penetration testing firm is selected for the later validation phase.
Phase 1 is also the right time to run a structured discovery workshop for startups if the product is at the idea or early-validation stage. The workshop converts a vision document into a buildable specification.
Phase 2: Architecture and Compliance Design
The tech lead and a security engineer produce the system architecture, the data flow diagram, the encryption scheme, the authentication and authorisation model, the audit log design, and the disaster recovery plan. A HIPAA risk assessment runs in parallel for US-bound systems.
The architecture document is reviewed with the client and, if the client has one, a third-party compliance auditor. Phase 2 ends with a signed architecture and a Business Associate Agreement (BAA) draft for the cloud provider. The architecture document is what the client will hand to a hospital security review or a payer due diligence team months later, building it well saves significant time downstream.
Phase 3: Iterative Build
Two-week sprints, each ending in a demo to the client. The team is typically 4 to 8 engineers: a tech lead, two to four backend engineers, one to two frontend or mobile engineers, a QA engineer, and a part-time devops engineer. The tech lead runs the standup, the sprint planning, and the retrospective.
The client product owner approves user stories. Compliance documentation is updated at the end of every sprint, not at the end of the project. This is a non-trivial discipline; it adds about 10% to development time and removes about 60% of the compliance retrofit risk at the end.
Phase 4: Compliance Validation and Penetration Testing
An independent penetration test runs against the staging environment. The compliance documentation is finalised: data flow diagrams, encryption inventory, access control matrix, audit log samples, incident response plan, and the risk register. For US-bound systems, this is the package a HIPAA auditor or a covered entity's security team will request before signing the BAA.
Phase 5: Production Deployment and Hyper-care
Production cutover is staged: a soft launch with a small clinician cohort, then a controlled rollout, then full release. Each step is gated on a defined set of operational metrics, error rate, support ticket volume, audit log integrity, that must hold before the next gate opens.
Hyper-care is a four to eight week period where the build team stays on the engagement to fix any production issues within agreed Service Level Agreement (SLA) windows. Most issues surfaced in hyper-care are workflow gaps rather than bugs: a clinical step the design did not anticipate, a report a billing team needs in a different format, an alert threshold that needs tuning.
After hyper-care, the engagement either rolls into a longer support contract through software support and maintenance services, or transitions back to the client's internal team with a documented handover.
The phase boundaries matter because they are also the cost boundaries. A client can pause the engagement at the end of any phase. This structure protects the client from sunk cost and protects the vendor from scope drift. It is the standard Acquaint Softtech delivery shape for healthcare work.
Quick Take
Builds run in five named phases: Discovery, Architecture, Iterative Build, Compliance Validation, Production & Hyper-care. Every phase has a signed deliverable and a clean pause point, which is how the model stays risk-adjusted for both sides.
Who Should Be on Your Healthcare Build Team

A common reason healthcare builds run over budget is that the team composition was modelled on a general SaaS build and only adjusted later. Healthcare needs roles that a SaaS team often does without, specifically a compliance lead, a clinical advisor, and a security engineer. Below is the team composition we deploy on most healthcare engagements at Acquaint Softtech, with allocations that hold for a 4 to 8 person team.
Role | Allocation | Owns | Typical Seniority |
Tech Lead | Full-time | Architecture, code review, sprint planning, BAA review, escalation point for the client. | Senior (8+ years) |
Backend Engineers | 2 to 4 full-time | API design, business logic, integrations, audit log infrastructure, background workers. | Mid to Senior |
Frontend / Mobile | 1 to 2 full-time | Patient app, clinician dashboard, accessibility compliance, role-specific surfaces. | Mid to Senior |
QA Engineer | Full-time | Functional, regression, and clinical workflow validation; test evidence trail for audit. | Mid to Senior |
DevOps Engineer | Part-time (50%) | Environment management, deployment pipeline, HIPAA-eligible cloud configuration, BAA implementation. | Senior |
Compliance Lead | Part-time (20-40%) | HIPAA risk assessment, audit log design, vendor BAA tracking, breach notification runbook. | Senior |
Clinical Advisor | Part-time (10-20%) | Workflow validation, clinical safety review, terminology mapping, change management with end users. | Domain expert |
Security Engineer | Part-time, intensive at launch | Encryption review, access control review, penetration test coordination, production hardening. | Senior |
Project Manager | Part-time (30%) | Sprint cadence, demos, status reporting, client coordination, change order tracking. | Mid to Senior |
The compliance lead, clinical advisor, and security engineer are the three roles most commonly missing from initial estimates. They are not optional in healthcare. Excluding them does not save money; it shifts the work onto the tech lead and the engineers, who are not trained for it, with predictable results.
At Acquaint Softtech, the compliance lead and the security engineer are bench resources we share across multiple healthcare engagements. The client pays for the percentage they actually consume rather than carrying a full headcount. The clinical advisor is usually engaged either through the client (preferred) or through a vetted third-party network; we do not staff in-house clinicians because clinical credibility lives with practising clinicians, not with a software firm.
How the Team Scales Through the Build
The team composition changes through the five phases. Phase 1 is heavy on the tech lead, the compliance lead, and the clinical advisor, code engineers are not yet involved. Phase 2 adds the security engineer and the DevOps engineer for the architecture work. Phase 3 ramps to full team size and stays there for the bulk of the build. Phase 4 brings the security engineer back for the penetration test cycle. Phase 5 narrows back to the tech lead, one or two engineers, and the DevOps engineer for hyper-care.
Capacity planning that assumes a flat 8-engineer team across all 30 weeks overpays in Phases 1, 2, and 5 and underpays in Phase 3. The phased shape is one of the levers that keeps the cost model honest.
If you need help scaling the team into your existing organisation rather than running it as a self-contained vendor team, our staff augmentation model embeds Acquaint engineers directly into your team under your management.
What Features Does Healthcare Software Need? (By Category)
"What features does healthcare software need?" is the second most common question we hear at the start of a build conversation, after "what does it cost?" The answer depends on the category. The table below summarises the must-have V1 features and the common V2/V3 features for each of the six categories, drawn from the Acquaint Softtech delivery archive.
Treat the V1 column as the minimum credible feature set for a production launch. Treat the V2/V3 column as the features that buyers commonly request in the first 6 to 12 months after launch, once initial usage data is in. Healthcare software features and architecture decisions are easier to defend when they are tied to specific user workflows rather than to a long generic checklist.
Healthcare Category | Must-Have Features (V1) | Common V2/V3 Features |
Telemedicine & Virtual Care | • Patient registration and intake forms • Clinician availability and booking • Waiting room and queue management • Encrypted video consultation (WebRTC) • Clinical notes and prescription writing • Payment collection and receipt • Post-visit summary and follow-up • Full audit log of every session | • EHR integration (FHIR R4) • E-prescribing (NCPDP SCRIPT in US) • Group or family consultations • Async messaging between visits • Multi-language support • Insurance eligibility check • Ambient AI scribing • Home blood-test ordering |
Electronic Health Records | • Patient demographics and chart • Encounters and clinical notes • Medications, allergies, problems • Lab and imaging results • Order entry (labs, imaging, referrals) • Clinician access controls (RBAC) • Full audit log per HIPAA • FHIR R4 export and import | • Multi-site practice management • Clinical decision support rules • Patient portal • Quality measure reporting (HEDIS, MIPS) • Voice-to-text dictation • AI-assisted note generation • Population health dashboards • Research data extracts (de-identified) |
Remote Patient Monitoring | • Device pairing and provisioning • Real-time vitals ingestion (BLE) • Clinician dashboard with alerts • Patient app with daily readings • Alert thresholds and escalation • CPT code event generation • Full audit log of access • Clinical care plan management | • Multi-device support (manufacturer SDKs) • Predictive risk scoring • Virtual care plan templates • Family/caregiver access • EHR integration (FHIR Device) • Automated billing event submission • Medicare/Medicaid reporting • Population analytics |
Hospital & Clinic Management | • Patient registration and master index • Appointment scheduling • Bed and resource management • Pharmacy and inventory • Clinical documentation • Billing and revenue cycle • Doctor and staff rosters • Regulatory reporting | • Lab and imaging integration (HL7/DICOM) • Mobile clinician apps • Advanced analytics and BI • Queue and emergency triage • Insurance pre-authorisation • Multi-specialty workflows • Integration with national health IDs • Telemedicine module add-on |
Pharmacy, Lab, & Diagnostics | • Prescription verification (pharmacy) • Drug interaction checks (pharmacy) • Sample tracking (lab) • Instrument interface (lab) • Result delivery (lab) • DICOM viewer (imaging) • Structured reporting (imaging) • Full audit log | • Controlled substance tracking (DEA) • PDMP integration (US) • Insurance claim submission • Barcoded sample chain of custody • AI-assisted result interpretation • Reference range customisation • Multi-site lab consolidation • PACS integration |
AI, Analytics, & Decision Support | • Clinician-facing recommendation UI • Explainability for every prediction • Confidence and uncertainty display • Audit log of every model output • Human-in-the-loop review queue • Fallback workflow when model is uncertain • A/B testing framework • Outcome measurement instrumentation | • Multi-model ensemble routing • Fine-tuning on local data • Federated learning across sites • Regulatory dossier generation (FDA SaMD) • Ambient scribe integration • Voice-driven clinical search • Multi-modal input (text + image) • Clinical trial matching |
This is a starting checklist, not a specification. The actual feature set for any specific product is a conversation between the product owner, the clinical advisor, and the tech lead. Acquaint Softtech runs that conversation as part of Phase 1 (Discovery), with the output being a prioritised feature backlog tied to the V1 launch criteria.
If the feature scope is uncertain or the product is at the early validation stage, our mvp development services practice is the right shape. The MVP scope deliberately covers the V1 column above and defers the V2/V3 column until the first cohort of users has validated the core workflow.
Quick Take
V1 is the minimum credible launch feature set; V2/V3 are the additions buyers request in the first 6 to 12 months once real usage data lands. Keep V1 narrow, ship, then iterate against measured behaviour.
What a Healthcare Software Build Includes: The Full Scope
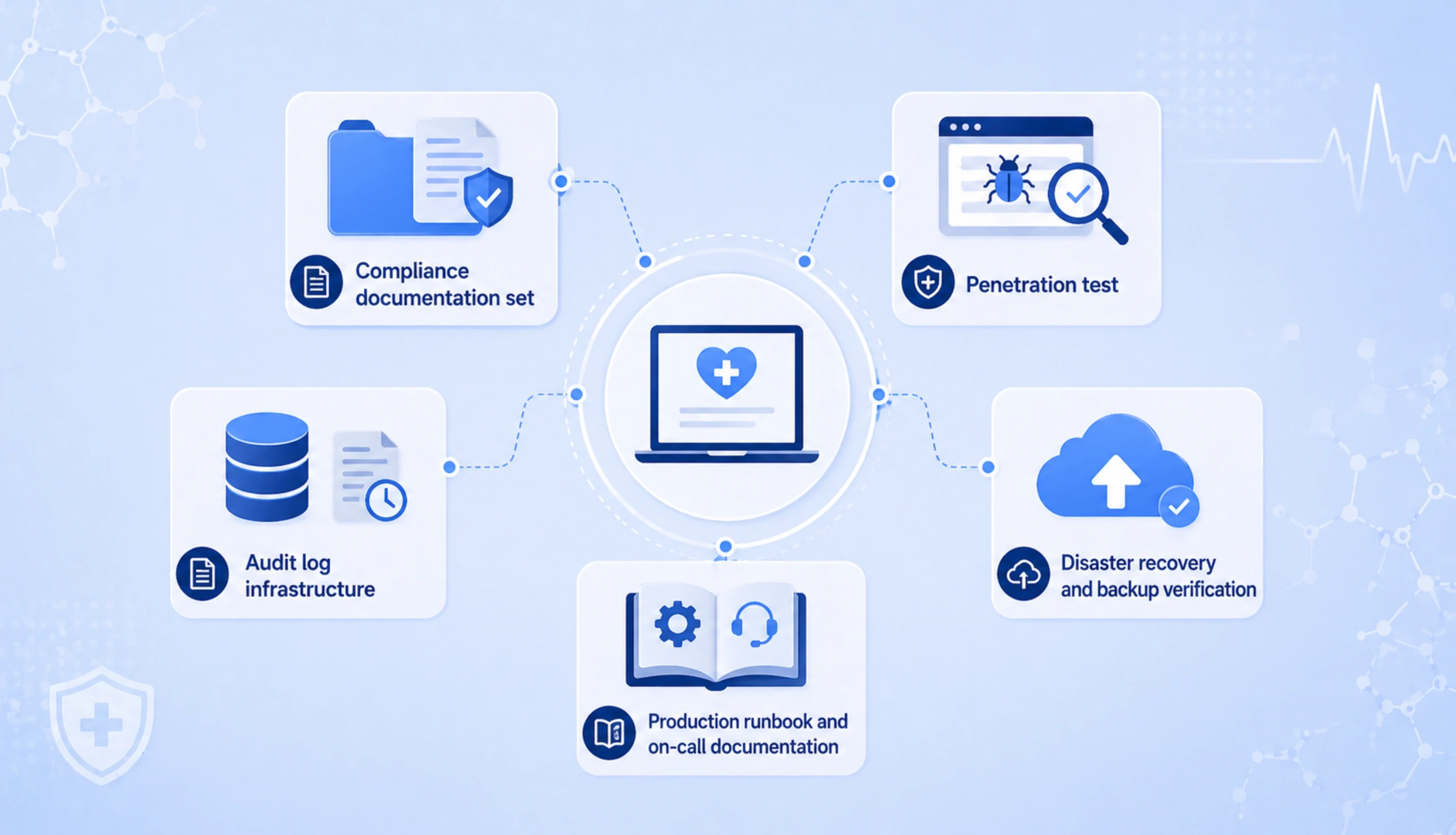
Healthcare clients sometimes receive build estimates that look attractive on a per-developer basis but exclude six items that are not optional in healthcare. Below is what every Acquaint Softtech healthcare build includes inside the quoted price, with no surcharge. The combined cost of these items, when added later as change orders, is usually 15 to 25 percent of the original build estimate.
Compliance documentation set
Data flow diagram, PHI inventory, encryption scheme document, access control matrix, audit log specification, incident response runbook, and the risk register. Maintained as live documents through the build, not assembled at the end. Each artefact is signed off by both the tech lead and the compliance lead at the relevant phase boundary.
Penetration test
An independent security firm runs a black-box penetration test against staging before production cutover. Findings are remediated by the build team. The penetration test report becomes part of the client's compliance evidence pack and is used in subsequent payer reviews and hospital security assessments.
Audit log infrastructure
Immutable, append-only audit logs covering every read, write, export, and administrative action on PHI. Default retention is six years to align with HIPAA. The audit query interface is built into the admin panel so a clinician or compliance officer can answer an access query without engineering involvement.
This is genuinely non-trivial volume. A mid-size clinic system processes 10 to 50 million audit events per month. The infrastructure has to handle that volume cheaply, query it in under a second for compliance officer requests, and survive any reasonable cloud failure scenario without losing events.
Disaster recovery and backup verification
Encrypted backups, tested restoration, and a documented Recovery Time Objective (RTO) and Recovery Point Objective (RPO). Backup restoration is exercised once during the build and the result is documented. This is what the client will be asked to demonstrate during a payer or hospital security review, "show us your last successful restore" is a standard question.
Production runbook and on-call documentation
A written runbook covering deploy procedure, rollback, common incident classes, escalation paths, and the on-call rotation. The runbook is the bridge between the build team and whichever team owns the system in steady state, whether that is Acquaint Softtech under a support contract or the client's internal operations team.
If a build estimate does not include these six items, they will be added later as change orders. The combined cost is usually 15 to 25 percent of the original build estimate. Acquaint Softtech includes them by default because in healthcare they are not optional features. They are the conditions of going to production.
For clients who have built a healthcare product but do not have these artefacts yet, our software version upgrade services practice includes a compliance retrofit programme.
What Does Healthcare Software Development Cost in 2026?

This section answers the most common question we receive from prospective clients. Healthcare software development cost 2026 varies by category, by jurisdiction, and by team model.
The table below shows the ranges Acquaint Softtech sees in active engagements as a healthcare software development company serving clients across the US, UK, Australia, and the UAE, separated by engagement size. All numbers are in US dollars per month for an offshore dedicated team based in India.
Equivalent in-house cost is calculated using the fully-loaded cost of an in-house engineer in San Francisco, including benefits, payroll taxes, recruiting, and overhead at roughly 1.4 times salary. The US Bureau of Labor Statistics OES data provides the underlying salary baseline.
Engagement Tier | Monthly Cost (USD) | Equivalent In-House (USA) | Annual Saving | Mgmt Overhead |
Small (3 to 4 engineers) | $13,000 to $20,000 | $60,000 to $80,000 | $564,000 to $720,000 | 1 to 2 hrs/wk |
Medium (5 to 8 engineers) | $22,000 to $36,000 | $100,000 to $160,000 | $936,000 to $1,488,000 | 2 to 4 hrs/wk |
Large (9 to 15 engineers) | $38,000 to $65,000 | $180,000 to $300,000 | $1,704,000 to $2,820,000 | 4 to 6 hrs/wk |
SAVINGS : Healthcare clients consistently save 40% or more by switching from US in-house hiring to an Acquaint Softtech dedicated team, without losing HIPAA, audit, or accountability discipline. |
What the monthly rate includes at Acquaint Softtech:
• All engineering hours within the contracted team capacity
• Tech lead time for sprint planning, code review, and architecture decisions
• QA engineer time for functional, regression, and compliance test execution
• Devops time for environment management and deployment pipeline maintenance
• Compliance documentation maintenance through the build
• Project management hours for sprint cadence, demos, and reporting
• Standard tooling: Jira, Git, CI pipeline, staging environment hosting
The rate the client pays is the rate. No additional employer overhead on top.
Penetration testing, third-party clinical advisor fees, and production cloud hosting are billed separately and pass-through, with no markup.
Want a Healthcare Build Estimate Grounded in Real Delivery Data?
Send us a one-paragraph description of the product you want to build. We send back a team structure, a phase plan, and a monthly rate within 48 hours. You interview the proposed tech lead before any engagement starts. No engagement begins without client approval of the team and the plan.
HIPAA and Healthcare Compliance: What the Code Actually Has to Do
Compliance is the area where briefs are vaguest and the cost of vagueness is highest. The clearest way to think about HIPAA and equivalent regimes is as a set of concrete engineering requirements rather than a policy document. This section walks through each of the seven engineering domains HIPAA touches, with the actual technical decisions a development team has to make in each.
Encryption
AES-256 for data at rest. TLS 1.3 for data in transit. Field-level encryption for the most sensitive PHI fields where the threat model justifies it, typically Social Security Numbers, full date-of-birth combinations, and any genetic or substance-use data.
Key management runs through the cloud provider's Key Management Service (KMS). Rotation policies are documented in the runbook. Customer-managed keys (where the client controls the master key, not the cloud provider) are the default for enterprise healthcare clients; provider-managed keys are acceptable for HealthTech startups where the cost of customer-managed keys outweighs the marginal security benefit.
Access control
Role-Based Access Control (RBAC) with the principle of least privilege as the default. Multi-factor authentication for every clinician and administrator account. Session timeouts appropriate to the workflow, typically 15 minutes for clinician workstations and 30 minutes for back-office roles.
Break-glass access procedures documented and audited, clinicians sometimes need emergency access to a chart they would not normally see, and the system has to support that without the workaround being an unaudited backdoor. Production engineering access is restricted to a named subset of the team and is logged with the same rigour as clinical access.
Audit logging
Every access to PHI is logged with user identity, timestamp, action type, and the record accessed. Logs are immutable and stored separately from the application database. Six-year retention is the HIPAA default; some state laws and clinical contexts (paediatrics, mental health) require longer.
The system provides a query interface for compliance officers to answer access questions without engineering intervention. "Who looked at patient X's record between dates A and B and why?" must be answerable in under a minute by the compliance officer through the admin UI, not an engineering ticket.
Audit log volume scales with usage and is genuinely large. A 10-clinician practice generates 50,000 to 200,000 audit events per day. A hospital generates millions. The infrastructure (an append-only store, a partitioned PostgreSQL table, or a managed service like AWS QLDB) has to be selected with that volume in mind from the architecture phase.
Engineer-side controls
Acquaint Softtech engineers who work on healthcare projects complete annual HIPAA awareness training and sign a confidentiality agreement covering PHI. Production access is restricted to a named subset of the team and is logged with the same audit rigour as clinical access. Background checks are run for engineers who will hold production access.
This is a contract term in any legitimate healthcare engagement, not a negotiation point. If a vendor declines to commit to engineer-side controls in writing, that is a meaningful signal about how seriously they take the rest of the compliance work.
All seven engineering domains above run as a parallel programme inside our end-to-end software product development engagements. Compliance is not a separate workstream we add at the end. It is sprint discipline, sprint after sprint, with documentation versioned alongside the code.
The Tech Stack Question: What to Build Healthcare Software In

This section is the healthcare software tech stack guide we hand to founders and CTOs at the start of every build. The right stack for a healthcare product depends on the category, the team you can hire and retain, and the integration surface. Below is what Acquaint Softtech sees most often across our healthcare delivery, with the trade-offs at each layer.
Backend: Laravel, Python, or Node.js
Laravel is our most-deployed backend for healthcare clinic systems, pharmacy platforms, and EHR-adjacent tools. The framework is mature, the ecosystem is well-documented, and the talent pool is deep. Acquaint Softtech is an Official Laravel Partner, which means we get early access to framework features and direct escalation to the core team for complex deployments.
Python (Django or FastAPI) is the right choice when the product has a significant analytics, AI, or device-data ingestion component. The Python ecosystem has the best healthcare-specific libraries: HL7apy for HL7 v2 parsing, fhir.resources for FHIR R4, pydicom for DICOM imaging, and the entire scientific Python stack for any analytics work.
Node.js fits real-time use cases such as telemedicine signalling, live dashboards, and any product where WebSocket-heavy traffic dominates. The healthcare-specific library ecosystem is thinner than Python's, but for a real-time-heavy product the runtime characteristics outweigh the library gap.
We compare these stacks in detail in our PHP versus Python versus Node.js for SaaS analysis, and the same trade-offs hold for healthcare with the addition of HL7 and FHIR library availability favouring Python and Java for deep EHR integration. If you need backend specialists, you can hire dedicated laravel developer or hire dedicated python developer profiles from us within 48 hours.
Frontend: React or Vue
React dominates clinician-facing dashboards and patient portals. Component libraries with WCAG 2.1 AA accessibility built in (Mantine, Chakra UI, MUI) are non-negotiable for clinician interfaces because clinicians use the system under time pressure and any usability friction translates directly into clinical risk.
Vue is a credible alternative for smaller teams that prefer its developer experience. The choice rarely matters for the user; it matters for the team you can sustain over the multi-year support window healthcare products require.
Mobile: React Native or native (Swift, Kotlin)
React Native is the default for patient-facing apps because the codebase is shared across iOS and Android and the development cost is roughly 60 percent of two native builds.
Native is the right choice when the app integrates deeply with device hardware. This includes Bluetooth Low Energy for connected devices, HealthKit and Health Connect for wearables, or frame-rate-critical UI such as live video consultation.
Database: PostgreSQL or a managed equivalent
PostgreSQL is the workhorse for healthcare clinical data. It supports JSONB for flexible record fields, strong transactional guarantees, and Row-Level Security for tenant isolation.
For high-volume time-series data from RPM devices, a time-series database is added alongside the primary database. TimescaleDB (a PostgreSQL extension) and InfluxDB are the common choices.
Hosting: AWS, Azure, or Google Cloud (HIPAA-eligible regions)
All three major clouds offer HIPAA-eligible services and will sign a Business Associate Agreement. The choice is usually driven by the client's existing cloud relationship, the available regional data residency, and the ecosystem fit for any AI workload. For UK and EU clients, data residency in-region is the governing constraint, and the NHS Data Security and Protection Toolkit sets the baseline supplier expectation for NHS-bound work.
If you need a stack-specific team, the Acquaint Softtech hire pages list the seniority bands and engagement models available. You can hire Laravel developers to build robust, scalable web applications tailored to your business needs.
For data-heavy or AI-driven projects, you can hire Python developers who bring deep expertise in backend systems, machine learning, and automation workflows.
If your product requires a cross-platform mobile presence, you can hire React Native developers to deliver seamless iOS and Android experiences from a single codebase.
To keep your infrastructure reliable, secure, and continuously deployed, you can hire DevOps engineers who specialize in cloud pipelines, containerization, and system observability.
Real-time + async architecture at scale
Our eLearning platform engagement runs the same dual-channel pattern healthcare needs: live virtual classrooms over WebRTC alongside an asynchronous API for course content, quizzes, and progress. The architecture transfers cleanly to telemedicine and any healthcare product that runs synchronous video plus asynchronous data over the same backend.
The 5 Questions That Tell You Whether to Build In-House or With a Partner
Most healthcare programmes do not need a binary in-house versus outsourced choice. They need an honest answer to five questions, after which the right model is usually obvious.
Has your team shipped a HIPAA or equivalent regulated build before?
Yes = your in-house team can lead the build with vendor support for capacity. No = a partner with healthcare delivery history is the lower-risk path, and the partner should provide the tech lead and the compliance lead.
Do you have engineering management capacity to run sprint planning, code review, and on-call for a 4 to 8 person team for the next 12 months?
Yes = staff augmentation works; you absorb engineers into your team and you manage them. No = a dedicated team is the right model; the vendor provides the management layer along with the engineers.
Is the build a one-off project or an ongoing programme?
One-off project = a fixed-scope engagement is reasonable. Ongoing programme = a dedicated team is the right structure because continuity matters more than scope precision.
How tight is your timeline?
Less than 6 months to first production release = an established partner with bench depth ships faster than a new in-house hire-and-build can. More than 12 months = either model works.
Is the product the core of your business or a supporting capability?
Core product = you want to own the codebase and operational knowledge long-term. Supporting capability = full outsourced delivery with a long-term maintenance contract is often the most economical model.
If three or more of the answers point toward partner involvement, the next decision is which partner shape fits.
Acquaint Softtech delivers both shapes. Our it staff augmentation services covers the embedded model, the right shape when you want to hire developers for healthcare software development and absorb them into your existing team. Our software development team covers the vendor-managed model, the right shape when you want to outsource healthcare software development to India end-to-end while keeping the codebase, the data, and the IP in your own jurisdiction. For pre-build clarification or interim CTO support, our virtual cto services practice provides a fractional senior technologist.
We Build the Team. You Interview Before You Commit.
Tell us your category (telemedicine, EHR, RPM, hospital management, pharmacy, or AI), your target jurisdiction, and your timeline. We send a team structure with named developer profiles within 48 hours. You interview before you commit. No engagement starts without your approval of the team.
Common Misconceptions About Healthcare Software Development
These five misconceptions show up in almost every first-call conversation Acquaint Softtech has with a new healthcare prospect. Each one, left uncorrected, leads to a predictable category of build failure later.
MISCONCEPTION : Off-the-shelf EHRs cover everything we need, so we never need custom software.
REALITY : Off-the-shelf EHRs cover the legal and clinical baseline. They rarely cover the workflow that makes a clinic, hospital, or HealthTech product distinctive. Most of our healthcare engagements are not EHR replacements; they are integrations, extensions, and workflow tools that sit alongside an EHR and use FHIR or HL7 to read and write the canonical record.
MISCONCEPTION : Offshore healthcare development is risky because of data residency.
REALITY: Data residency is a configuration decision, not a vendor location decision. Acquaint Softtech engineers based in India routinely build systems where the production data, the staging data, and even the development environments are hosted in US, UK, EU, or UAE regions per the client's regulatory requirement. Engineering access is controlled through identity and audit, not geography. We cover the operational pattern in detail in our analysis of red flags when outsourcing development.
MISCONCEPTION : We can hire one healthcare engineer in-house and they will figure out the rest.
REALITY : A single healthcare engineer, even a senior one, cannot replace the team composition healthcare requires. The compliance lead role, the security engineer role, the clinical advisor role, and the QA discipline are all distinct from "the engineer who writes the code." The right pattern for a small team is to add a senior engineer in-house and supplement with vendor-provided compliance, security, and clinical advisory bench resources for the percentage of time those roles actually consume.
If you have heard one or more of these from another vendor or from internal stakeholders, treat it as a signal that the conversation needs more depth before any commitment.
Ourvirtual services practice exists for exactly this kind of pre-build clarification engagement, where the deliverable is a signed-off architecture and compliance plan rather than code. For pre-revenue HealthTech founders specifically, our software development outsourcing for startups engagement model bundles the architecture, the compliance documentation, and the build into a single accountability structure rather than three separate vendors.
See What a Healthcare Software Build Looks Like for Your Product
Send us your category, your jurisdiction, and a paragraph on the workflow you want to digitise or replace. We respond within 48 hours with a phase plan, a team structure, and a monthly rate. You interview the proposed tech lead before any engagement starts.
-
How much does it cost to build healthcare software?
A focused HIPAA-aligned healthcare MVP built with an offshore Acquaint Softtech team typically lands between $80,000 and $200,000 for the build phase, depending on the category and the integration surface. Telemedicine is usually at the lower end. A full-featured healthcare software build with EHR integration, multi-specialty support, and AI features sits between $200,000 and $600,000 depending on category.
-
What features does healthcare software need?
The features depend on the category, but every credible healthcare software build needs eight foundational capabilities: secure authentication with multi-factor support, role-based access control, encrypted data storage and transmission, an immutable audit log of every PHI access, a clinical workflow appropriate to the user role, integration with at least one external clinical system through HL7 or FHIR, regulatory reporting outputs, and a backup and disaster recovery process with documented Recovery Time Objective and Recovery Point Objective.
-
How long does a healthcare software MVP take to build in 2026?
A focused healthcare MVP typically takes 16 to 24 weeks to first production release, compared with 8 to 12 weeks for a general SaaS MVP. The added time is the compliance programme that runs in parallel: architecture review, HIPAA risk assessment, audit log design, and the penetration test before cutover.
-
What is the difference between HIPAA, GDPR, and the UK NHS Data Security and Protection Toolkit?
HIPAA is the US federal regulation governing PHI handled by covered entities and their business associates. GDPR is the EU regulation governing all personal data including health data. The NHS Data Security and Protection Toolkit is the UK NHS-specific assessment that suppliers must complete to handle NHS data.
-
Can we outsource healthcare software development to an offshore team without violating compliance?
Yes, when the engagement is structured correctly. The cloud region holds the data, not the developer. Acquaint Softtech routinely builds healthcare systems where the data, the staging environments, and the production environments are all hosted in the client's required jurisdiction while the engineering team is in India.
-
What happens to the codebase and the data if the engagement ends?
The codebase belongs to the client from day one. It is hosted in the client's repository, or in a repository we transfer to the client at any point on request. At the end of an engagement, the build team produces a written handover including the architecture document, the runbook, the compliance documentation, and a knowledge transfer session for whichever team takes over operations.
-
How do we handle clinician workflow validation if our team is in a different time zone from our developers?
Clinician workflow validation runs as scheduled sessions, not as informal back-and-forth. Acquaint Softtech overlaps four to five hours per day with US Eastern, US Pacific, UK, and Australian working hours, depending on the engagement. Demos, sprint reviews, and clinical advisor sessions are scheduled inside the overlap.
-
Is a dedicated team appropriate for a pre-revenue HealthTech startup?
Yes, in most cases, because the alternative for a pre-revenue startup is usually a freelance team that costs less per hour but lacks the compliance discipline that healthcare requires. A dedicated team of 3 to 4 engineers from Acquaint Softtech costs $13,000 to $20,000 per month all-in, which is below the fully-loaded cost of one mid-level US healthcare engineer.
-
What tech stack is best for healthcare software in 2026?
There is no single best stack. The most common stack we deploy at Acquaint Softtech for healthcare in 2026 is React Native or Flutter for the patient mobile app, React for the clinician web app, Python (Django or FastAPI) or Laravel for backend services, PostgreSQL with field-level encryption for the data layer, and AWS, Azure, or Google Cloud in a HIPAA-eligible region for hosting.
-
Can we build the patient app and clinician app on the same codebase?
Technically yes, practically no. The clinician workflow (queue management, multi-patient context, EHR access, prescription writing, billing handoff) is fundamentally different from the patient workflow. The right pattern is two apps that share the same backend services and data layers but present role-specific surfaces.
Table of Contents
Get Started with Acquaint Softtech
- 13+ Years Delivering Software Excellence
- 1300+ Projects Delivered With Precision
- Official Laravel & Laravel News Partner
- Official Statamic Partner
Related Reading
Custom Healthcare Software Development: An End-to-End Guide
Custom healthcare software is revolutionizing the medical industry by providing tailored solutions that enhance patient care, streamline processes, and improve security. Discover the benefits, challenges, and step-by-step guide to building effective custom healthcare software. Learn how expert developers can help you stay ahead in the evolving healthcare landscape.

Mukesh Ram
February 27, 2025Healthcare & IT Staff augmentation - A success partnership
Healthcare IT staff augmentation bridges skill gaps and reduces workloads by hiring remote developers. This strategy enhances IT capabilities, ensuring smooth implementation and management of advanced technologies in healthcare organizations.

Mukesh Ram
August 6, 2024Proof of Concept: Why is it important in software development?
Discover how a Proof of Concept (PoC) can validate your project's feasibility, enhance stakeholder trust, and streamline development processes effectively.

Acquaint Softtech
April 28, 2025India (Head Office)
203/204, Shapath-II, Near Silver Leaf Hotel, Opp. Rajpath Club, SG Highway, Ahmedabad-380054, Gujarat
USA
7838 Camino Cielo St, Highland, CA 92346
UK
The Powerhouse, 21 Woodthorpe Road, Ashford, England, TW15 2RP
New Zealand
42 Exler Place, Avondale, Auckland 0600, New Zealand
Canada
141 Skyview Bay NE , Calgary, Alberta, T3N 2K6



